Acmeware Achieves 100% Submission Success
Featured article
Acmeware completes 100% successful submissions for eCQM, PQRS, Hospital IQR, and Joint Commission ORYX using OneView for acute and ambulatory settings.
The CY 2023 OPPS Proposed Rule addresses the Hospital OQR Program with measure, timing, and validation changes.
Article content
CMS recently released the CY 2023 OPPS Proposed Rule, which included proposals for the Hospital Outpatient Quality Reporting Program (OQR) Program. For the full text of the rule, see the Federal Register.
The OP-31 measure has been a voluntary reporting measure but was previously finalized as mandatory beginning with the CY 2025 reporting period. In this rule, CMS proposes to remove the mandatory requirement and continue to make OP-31 a voluntary measure.
Since the removal of OP-26, the Hospital OQR Program does not capture outpatient surgical procedure volume in hospitals. CMS is considering reimplementing OP-26 measure or another volume measure because the shift from the inpatient to outpatient setting has placed greater importance on tracking the volume of outpatient procedures.
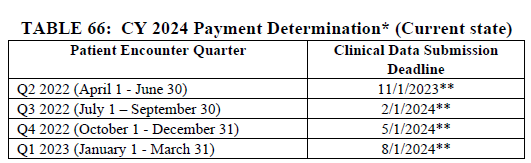
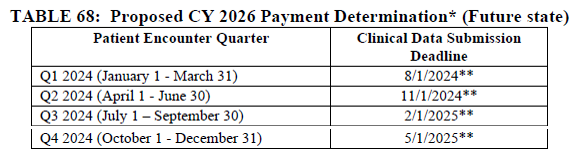
CMS is proposing to align the patient encounter quarters for chart-abstracted measures with the calendar year beginning with the CY 2024 reporting period (CY 2026 payment determination). If finalized, all four quarters of patient encounter data for chart-abstracted measures would be based on the calendar year two years prior to the payment determination year. This proposal will align the patient encounter quarters for chart-abstracted measures with those of the Hospital IQR program.
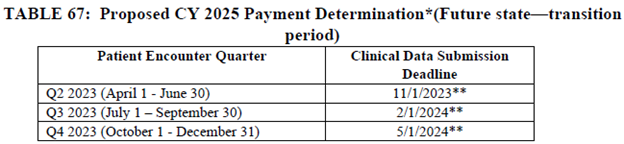
To transition to this proposed timeframe, CMS is proposing to only use three quarters of data for chart-abstracted measures for the CY 2023 reporting period (CY 2025 payment determination).
For validation purposes, CMS selects a random sample of 450 hospitals and selects an additional 50 hospitals based on targeting criteria. Beginning with validation affecting the CY 2023 reporting period (CY 2025 payment determination) CMS is proposing to add a fifth criterion to the targeting criteria for hospitals receiving Extraordinary Circumstances Exceptions with confidence intervals less than 75%.
If you have questions about reporting your OQR measures, please contact us.